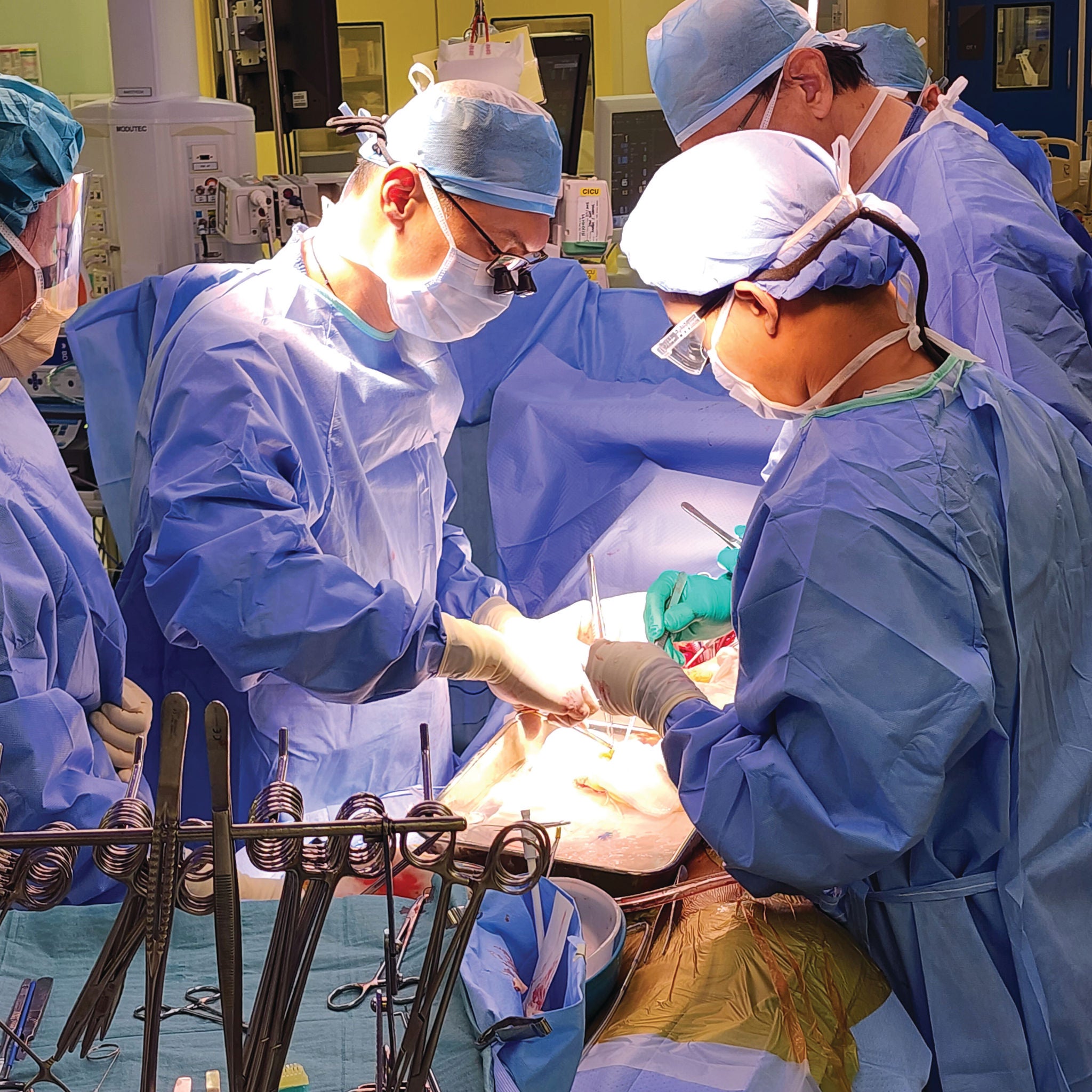
NHCS marks a remarkable milestone this year - 35 years of giving patients new leases of life through heart transplantation. As Singapore's only centre to carry out heart transplantation, NHCS has transformed the lives of over 100 patients, many of whom have gone on to lead fuller, more meaningful lives.
Since establishing the heart transplant programme in 1990, NHCS has grown to become the national referral centre offering end-to-end advanced heart failure care. The centre's comprehensive heart failure programme includes diagnostic tests and advanced therapies, from implantable cardiac devices that serve as either bridge-to-transplant or destination therapy, to heart transplantation.
"This year, we proudly celebrate the 35th anniversary of heart transplantation at NHCS," said Assistant Professor Tan Teing Ee, Deputy Chief Executive Officer and Director of Heart Transplant & Mechanical Assist Device Programme. "This milestone honours the exceptional dedication of our multidisciplinary team. Their collective expertise has driven our programme's success, most notably in our ventricular assist device (VAD) programme, improving patient survival rates for patients awaiting heart transplant from zero at 2 years to over 75% at 5 years. This incredible journey has transformed countless lives by turning advanced technology into lasting hope."

From Surgery to Systems
The first heart transplant in Singapore was performed in July 1990. At the time, patients with advanced heart failure faced limited treatment choices once conventional therapies were exhausted. The transplant programme was a leap forward in local cardiac care, revolutionising treatment options for patients with end-stage heart failure. The introduction of mechanical circulatory support devices in 2001 offered a bridge-to-transplant for heart failure patients. Subsequent breakthroughs, such as the implantation of the HeartMate II™ in 2009, the first HeartWare HVAD™ in 2012, and the HeartMate 3™ in 2015, have significantly improved patient outcomes, by making safer options available to more patients.
These life saving devices, also known as Left Ventricular Assist Devices (LVAD), are small mechanical pumps designed to take over the pumping function of the heart's main chamber that is the left ventricle, allowing blood to circulate effectively through the body. Implantation is done through an open-heart surgery. Since 1990, NHCS has performed 103 heart transplants and 156 VAD implants. By pioneering numerous firsts in the region, the heart transplant programme has achieved milestones that reflecting surgical, technological, and service delivery advancements.

Evolution of mechanical circulatory support devices(pump weights shown):
(1) HeartMate I Left Ventricular Assist System (LVAS) - 1.25 kg
(2) Thoratec Paracorporeal Ventricular Assist Device (PVAD) - 417 grams
(3) HeartMate IITM Left Ventricular Assist Device (LVAD) - 390 grams
(4) HeartWare HVADTM System - 160 grams
(5) HeartMate 3TM LVAD - 200 grams
More Than Just a Pump
While heart transplantation remains the gold standard for treating end-stage heart failure, mechanical circulatory support has become an equally critical pillar of care. Left Ventricular Assist Devices (LVADs), with models such as the HeartMate II™ and HeartMate 3™, allow patients to walk, climb stairs, work full-time, and even travel. Unlike early generations, today's devices are compact, silent, and can be worn discreetly to give patients a new sense of normalcy. The HeartMate 3™ features magnetically levitated rotor blades that reduce wear and virtually eliminate internal clotting.
With LVADs significantly improving survival rates, the average waiting time on the wait list for a transplant in Singapore has increased from about 150 days before LVADs to over 1,170 days today. For many patients, especially those who may not be suitable for transplant due to age or comorbidities, LVADs can be a destination therapy. "Patients who once had only months to live are now thriving for years. Some have gone back to school, started families, or returned to work. These are outcomes we only dreamed of 20 years ago," shares Kerk Ka Lee, Senior Clinical Transplant Manager, at Mechanical Circulatory Support, Heart & Lung Transplant Unit.
Behind every transplant or LVAD patient is a 24/7 multidisciplinary team. Surgeons, cardiologists, transplant coordinators, physiotherapists, pharmacists, medical social workers, and others come together to support each individual. Patients are guided through every stage from pre-surgery assessments to rehabilitation and on-going follow-ups. Activities like dental extractions or gym routines are carefully planned to ensure patient safety, reflecting the complexity and commitment required in long-term heart failure care.
Expanding the Transplant Pool, Enhancing Survival
Historically, certain conditions like Hepatitis B and HIV excluded patients from transplant consideration. Today, multidisciplinary collaboration with infectious disease specialists and the availability of potent antiviral and antiretroviral medications have made transplantation safe and feasible for many of these individuals.
Looking Forward
Next-generation pumps, wearable sensors, remote monitoring, and future possibilities such as xenotransplantation (transplantation of organs from one species to another) and genetic therapies are shaping the future of advanced heart failure treatment. Ongoing clinical research and collaborations aim to enhance long-term outcomes and reduce device-related complications. As NHCS commemorates 35 years of heart transplantation in Singapore, it remains committed to its mission to advance heart failure care, one heartbeat at a time.

Just the Numbers (as of July 2025)
• Longest ongoing LVAD bridge-to-transplant: 9 years
• Longest LVAD survival (destination therapy): 12+ years
• Youngest LVAD recipient in Southeast Asia: 13 years old
• Heart transplants performed: 103
• Mechanical heart (continuous-flow VAD) implants: 156
• Average waiting time for patients on current waitlist: 1,172 days
Keep Healthy With
© 2025 SingHealth Group. All Rights Reserved.



















