Radiological Sciences services within the SingHealth cluster are spread across 7 hospitals and national specialty centres, making it the largest radiology affiliation in Singapore, comprising 50% of public sector radiologists and nuclear medicine physicians. We provide extensive imaging and image-guided intervention services using modern imaging such as Computed Tomography (CT) and Magnetic Resonance Imaging (MRI), thus providing specialised services to our patients. Every year, we perform more than 1.3 million imaging studies and over 12,000 image-guided interventions. The nuclear medicine (NM) and molecular imaging service in SingHealth performs more than 17,000 NM and PETCT scans every year, with over 5000 clinic consultations and radionuclide treatments annually.
In 2021, Radiological Sciences SingHealth (RSS) was set up as a special unit within SingHealth to enhance the current radiological services by implementing patient-centric seamless care with innovation. This enterprising endeavour of the RSS involves integrating SingHealth imaging appointment slots island-wide into a central pool to ensure that our patients get their investigation and treatment as promptly as possible. Thus, patients may be directed to another SingHealth institution, other than their treating institution, to receive their imaging appointment. This allows patients to have their scan at the earliest availability, and when available, to book an appointment slot at a SingHealth institution closer to their home for greater convenience and accessibility. Imaging services across SingHealth institutions share a common set of treatment protocols and patients remain assured that high standards of care are consistently upheld across all our institutions.
Across the world, as in Singapore, Diagnostic Radiology uses various medical imaging techniques and equipment to help in the diagnosis of diseases. Radiologists are medical doctors who are trained to interpret radiographs, ultrasound, Computed Tomography (CT), Magnetic Resonance Imaging (MRI) and other scans to come to an accurate diagnosis, while nuclear medicine physicians are medical doctors who specialise in nuclear medicine molecular imaging (e.g. SPECT and PET) and therapy, so that the primary care team can make plans for treatment. Our radiologists and nuclear medicine physicians ensure that the most appropriate scan is performed for the patient’s problem and direct radiographers or nuclear medicine technologists to obtain good quality images.
SingHealth institutions provide a full range of diagnostic imaging examinations and image-guided interventions. Some common services are listed below.
Imaging Services
General radiography or X-ray
General radiography or x-ray is the foundation of all diagnostic imaging using ionising radiation. This technology uses x-rays to produce an image, which is captured by an image receptor. Plain radiographs are commonly requested by doctors as an initial evaluation upon first consultation or as baseline screening. X-rays may be taken in the x-ray rooms, or at the bedside when necessary.
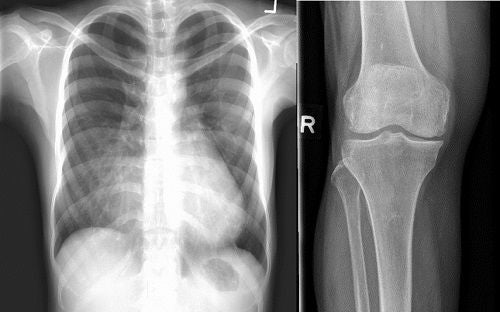
X-ray images courtesy of Sengkang General Hospital.
Fluoroscopy
Fluoroscopy uses a special contrast dye and a continuous stream of x-rays to produce images through which the radiologist can see the body part and its motion in detail. This provides the radiologist with information about the function and movement of the body in real time, which helps them to determine the appropriate diagnosis and treatment for the patient.
Examples of fluoroscopy investigations are: barium-related studies such as barium meal, barium enema, defecating proctography, and video fluoroscopy studies to assess swallowing abnormalities. Water-soluble contrast studies are popular in children and babies to look for congenital gastro-intestinal or urological abnormalities in studies such as water-soluble swallow, micturition cystouretherogram (MCU) etc. Water-soluble contrast scans are also performed in adults, mostly to look for post-surgical status or complications.
Fluoroscopy is also widely used in musculoskeletal imaging whilst performing diagnostic contrast injections for shoulder, wrist and hip joints prior to MRI. Therapeutic joint injections are occasionally performed using fluoroscopy, as are other procedures such as endoscopic retrograde cholangiopancreatography (ERCP), feeding tube insertions, fracture fixations using plates and screws etc.
Intravenous Urography
Intravenous urography is a specialised x-ray examination of the urinary system, including the kidneys, ureters and bladder. A contrast agent (dye) is injected before the scan, and is used to highlight the urinary tract and study the ability of the urinary system to excrete urine. In this procedure, the contrast agent injected into the body will be cleared by the kidneys and excreted out as part of the urine.
Patients are given instructions on how long to fast before the test. Diabetic patients should inform the radiography department before the scan as they may need different instructions on the preparations.
Computed Tomography (CT)
Computed tomography, commonly known as CT scans, combines the use of x-rays and computer systems to generate cross-sectional images of the human body. X-rays that pass through the body are captured and processed by the computer to create clear and detailed images of internal organs and structures. Advances in technology allow the x-ray dose to be tailored to each patient and kept as low as possible.
For certain types of scans, contrast (a special dye) is injected into the body to allow major blood vessels as well as organs to be seen more clearly.
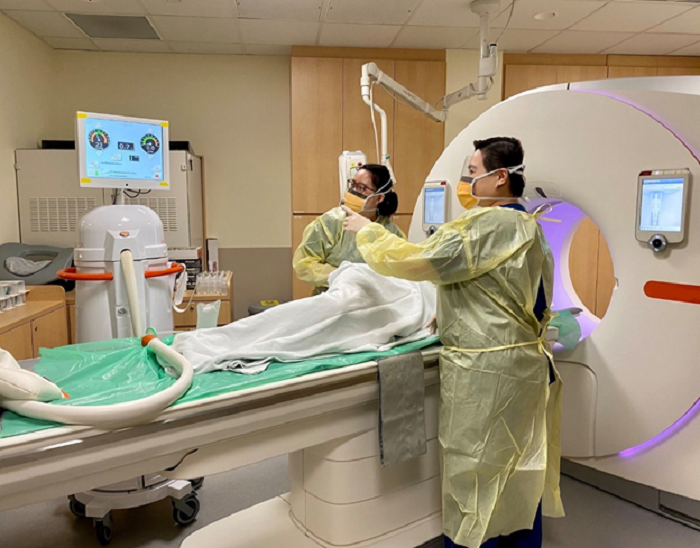
CT Colonography. Photo courtesy of Singapore General Hospital.
Bone Mineral Densitometry (BMD)
Bone Mineral Densitometry (BMD) is also known as Dual X-ray Absorptiometry (DXA). It is used to screen for reduced bone densities, also known as osteopenia or osteoporosis, and predict fracture risk. BMD can be used to monitor patients who are on treatment for such conditions.
BMD may also be used to measure body composition, i.e. the amount of bone, fat and muscle in the body, as part of clinical evaluation for patients who are obese or have muscle wastage. BMD involves a low level of radiation, much lower than standard X-ray examinations.
Angiography
Angiography is the x-ray imaging of blood vessels using contrast agents (dyes) injected into the bloodstream through a thin plastic tube or catheter that is placed directly in the blood vessel, to take images known as angiograms.
Angiography provides information about blood vessel abnormalities, such as narrowing, blockage, inflammation, abnormal widening and bleeding. The contrast agents are injected into the blood vessels to make them visible on X-rays. Angiography is also used to guide procedures that treat blood vessel abnormalities, such as inserting stents.
Breast imaging
SingHealth hospitals offer screening mammography, breast ultrasound, breast MRI and breast biopsies. A mammogram is a low-dose x-ray of the breasts to screen for breast abnormalities, especially useful for early breast cancer detection. Mammography may be used with other imaging techniques such as ultrasound and MRI to make a more accurate diagnosis. Breast ultrasound uses sound waves to create images of the internal structures of the breast, whilst breast MRI creates images of higher resolution. Breast biopsies are performed to remove a small amount of breast tissue for testing. Breast imaging services are offered at SGH, CGH, NCCS, KKH and SKH.
Magnetic Resonance Imaging (MRI)
SingHealth hospitals and specialty centres also offer scans without radiation, such as Magnetic Resonance Imaging (MRI), which uses a strong magnetic field and radio waves to take detailed images of organs and tissues in different planes of any part of the human body. This allows radiologists to visualise internal structures, especially soft tissues, in the body.
We perform a wide variety of MRI exams such as brain, spine, prostate, cardiac, breast and musculoskeletal MRI. Unlike x-rays or CT scans, MRI does not use radiation by default. Intravenous contrast dye may be used, which improves clarity of the images to make a more accurate diagnosis.
The strong magnetic field used in MRI attracts magnetic objects, including implants, jewellery and metal zippers which need to be removed prior to scanning. Please inform the radiographer if you have any metal implants.
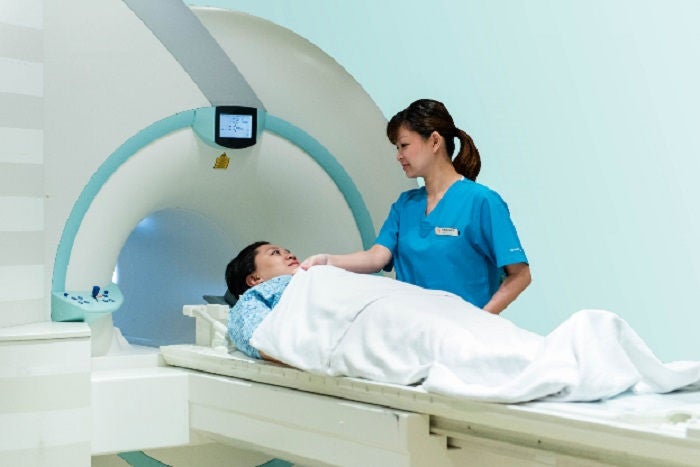
Magnetic Resonance Imaging (MRI). Photo courtesy of Sengkang General Hospital.
Ultrasound
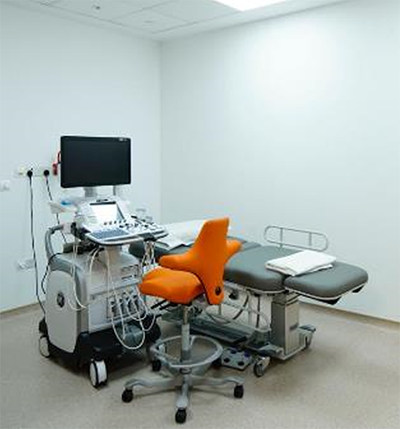
Ultrasonographic equipment. Photo courtesy of Sengkang General Hospital.
An ultrasound scan uses high-frequency sound waves to examine structures in the body, including large organs, blood vessels, muscles, tendons and ligaments. A scanning probe is placed on the skin which gives off high-frequency vibration, which enter the body and echo back, creating real time ultrasound images. Ultrasound does not involve radiation, and is a relatively safer imaging technique compared to common scans involving radiation. It is non-invasive and can be used safely in children and pregnant women.
Interventional Radiology
Interventional Radiology is a branch of medicine specialising in the use of modern imaging modalities, including digital subtraction angiography, ultrasound fluoroscopy and computed tomography (CT), to guide the performance of minimally invasive diagnostic procedures and treatments in different parts of the body. These treatments offer less risk, less pain and faster recovery, compared to traditional surgery.
Procedures done by our interventional radiologists include angiography, stent insertion, embolisation, biopsies and drainages, tumour ablation, and more.
Radiation Doses for Common Examinations
The scans and treatments described above use radiation to see inside the body. One of the most common concerns shared by patients in the Radiology department is "How much radiation is involved?"
Effective radiation dose is measured in milli-sieverts (mSv). We are exposed to natural background radiation daily, which is approximately 2.4mSv yearly. This figure varies depending on geographical location, as it depends on the radioactive elements in the air or the radioactive materials present in rocks, soil, or building materials. Nevertheless, we can estimate the effective radiation dose by comparing the average radiation dose from common scans with the dose that we receive daily from background radiation.
The effective doses of a few common examinations are:
| Examples of Common Scans | Approximate Effective Radiation Dose (mSv) | Comparable to natural background dose of: | |
|---|---|---|---|
| X-ray | Chest | 0.05 | 8 days |
| Abdomen | 0.50 | 2.5 months | |
| Pelvis & hip | 0.37 | 1.9 months | |
| Cervical spine (upper back) | 0.05 | 8 days | |
| Lumbar spine (lower back) | 0.80 | 4 months | |
| CT | Head | 1.7 | 8.6 months |
| Chest | 7.0 | 3 years | |
| Abdomen | 6.8 | 2.9 years | |
| Pelvis | 7.4 | 3.1 years | |
| Spine | 7.0 | 3 years | |
| *Please note that the effective doses listed above are typical values for an average-sized adult. The actual individual dose can vary substantially, depending on a person's size and the differences in imaging practices. This chart attempts to simplify a very complex topic, and hence it can only provide an estimation of the doses for each examination. | |||
Radiation and Pregnant Women
Radiation exposure by pregnant women is avoided as much as possible as it affects the foetus. The increased risk depends on the amount and duration of radiation to the foetus. The radiation risk is highest during the first few weeks of pregnancy, as the foetus is most sensitive during this development stage. Radiation risk decreases as the pregnancy progresses, and is relatively low when the foetus is fully developed, when birth defects due to radiation exposure are not likely to occur.
From past studies, the radiation dose from diagnostic examinations currently presents no risk of causing foetal death or problems in development. For most diagnostic medical procedures where the foetal dose is up to 1 mSv, the associated risk of childhood cancer due to radiation is very low (below 1 in 10,000) compared to the natural risk (approximately 1 in 500).
Even though most radiological examinations result in a low foetal dose, pregnant patients should avoid scans with radiation as far as possible, due to the small risk they have. Diagnostic radiological procedures or examinations are usually recommended during pregnancy when the information gained from the study is necessary for the care of the patient and when information cannot be obtained by other means, especially by ultrasound or MRI.
| Type of Scan | Typical foetal dose range (mSv) | Risk of childhood cancer per examination | |
|---|---|---|---|
| X-ray | Skull | 0.001 – 0.010 | <1 in 1,000,000 |
| Chest | |||
| Thoracic Spine | |||
| Head and/or neck | |||
| X-ray | Abdomen | 0.1 – 1.0 | 1 in 100,000 to 1 in 10,000 |
| Pelvis | |||
| Hip | |||
| CT | Chest & Liver | ||
| CT | Lumbar Spine | 1.0 - 10 | 1 in 10,000 to 1 in 1,000 |
| Abdomen | |||
| CT | Pelvis | 10 - 50 | 1 in 1,000 to 1 in 200 |
| Pelvis & Abdomen | |||
| Pelvis, Abdomen & Chest | |||
| *Foetal doses derived from doses to the uterus seen in UK surveys and Administration of Radioactive Substance Advisory Committee (ARSAC) Notes for Guidance, applied to early stages of pregnancy when the foetus is small. | |||
While exposure to radiation carries a certain amount of risk to the foetus, however, there are times when radiological examination would be the preferred way to obtain essential diagnostic information of the pregnant patient. Diagnostic scans with x-rays or CT have proven to be efficient and holistic in providing information about a patient’s internal injuries or conditions, especially for life-threatening cases.
Thus, the radiological examination will need to be performed as it is deemed necessary and carries greater benefit than risk to the pregnant patient. In such a case, it would be clinically justified to carry out radiological examinations for pregnant patients.
If there is a chance the patient is pregnant, our staff will discuss the benefits and risks of any radiological scans with the patient.
Lead Aprons and Shields for safety in Fluoroscopy / Interventional Radiology
You may notice our staff wearing a lead gown when attending to your scan. Fluoroscopy or interventional radiology (IR) procedures require clinical staff to be inside the room with patients when x-ray exposures are made continuously. Hence, our staff are required to protect themselves from radiation exposure by wearing lead aprons, thyroid shields and lead glasses, which are the standard shields commonly used to protect both staff and patients from unnecessary radiation exposure. The appropriate shielding reduces the amount of radiation exposure received by the body tremendously.

Staff donning a lead gown
Information on radiation dose and protection compiled by Laurentcia Arlany, Medical Physicist, Sengkang General Hospital.
Sources:
- J Vilar-Palop et. al. Updated effective doses in radiology. J. Radiol. Prot. 2016; 36:975-990
- B K Cheon et.al Radiation safety: a focus on lead aprons and thyroid shields in interventional pain management. Korean J Pain 2018; 31:244-242
- Centre for Disease Control and Prevention Radiation Emergency Fact Sheet, Radiation and Pregnancy: A Fact Sheet for the Public, 2011
- Guidelines for perinatal care. 3d ed. Elk Grove Village, Ill.: American Academy of Pediatrics and American College of Obstetricians and Gynecologists, 1992:210-3
- Protection of Pregnant Patients during Diagnostic Medical Exposures to Ionising Radiation, Health Protection Agency, The Royal College of Radiologists, 2009\
Preparations for scans and interventional procedures
Some scans and procedures involving x-rays or ionising radiation may not be suitable for pregnant patients. Do inform your doctor if the patient may be pregnant. The doctor will carefully weigh the benefits and risks before proceeding with the scan.
Some scans may require specific preparations, such as taking certain medicines, or fasting before the scan. Our care team will inform you of these beforehand. Do ask our care team in advance if you have any queries or concerns about the scans.
Diagnostic Radiology and Interventional Radiology services are available at:
Singapore General Hospital, Division of Radiological Sciences
Department of Diagnostic Radiology, Department of Vascular and Interventional Radiology and Radiography Department.

Department of Diagnostic Radiology, SGH.
As a 1,500-bed hospital, SGH houses the largest Radiology Department in Singapore and owns and operates over 100 pieces of imaging equipment. Being the largest hospital in Singapore with a large catchment area, it is a tertiary/ quaternary hospital centre, recently ranked 3rd in the world in 2019 and 8th in the world in 2020.
Radiology at SGH emulates the vision of: Illuminating lives through excellence in medical imaging. Patients, at the heart of all we do.
Dr Jeffrey Fong from SGH says, “The people in SGH are its biggest asset. All of the people here, from the doctors to the nurses, radiographers and other ancillary staff, are all keen to make a difference to the patient’s care, as epitomised by the vision above.”
In keeping with its tradition of teaching, Radiology at SGH conducts at least 16 multidisciplinary rounds where trainees and residents are strongly encouraged to attend and participate. This is very useful as it allows the trainees to hear the clinical needs perspective from our radiology work and is a conduit for frank interaction and discussion. SGH also participates in the larger SingHealth Division grand rounds held once a month.
For Radiology appointments at SGH, call (65) 6789 8883 or visit https://for.sg/rc to submit your details.
Changi General Hospital, Department of Diagnostic Radiology & Department of Radiography

Photo courtesy of Changi General Hospital.
The Department of Diagnostic Radiology in Changi General Hospital (CGH) serves over a million residents in eastern Singapore as a >1000-bedded hospital. There are more than 130 consultation rooms for specialist outpatient care and minor surgery rooms within its Medical Centre.
CGH is home to the largest multidisciplinary Sports & Exercise Medicine Centre in Singapore, using modern diagnostic technology such as bedside musculoskeletal ultrasound sonography and MRI.
CGH developed and implemented an award-winning Artificially Intelligent Work Distribution System in RIS, is an HIMMS Asia Pacific Elsevier Digital Healthcare Award 2016ding ICT Innovation Category Finalist, National Health IT Excellence Awards 2017 (Cat B – IT Excellence: Beyond Quality to Value) winner as well as houses award-winning faculty in Radiology Residency Education.

Awardees at the National Health IT Excellence Awards 2017. Photo courtesy of Changi General Hospital.

Radiographers’ Team Building. Photo courtesy of Changi General Hospital.
For appointments at CGH, call (65) 6788 8833.
Sengkang General Hospital, Department of Radiology

The SKH campus. Photos courtesy of Sengkang General Hospital.
As the newest restructured hospital in the SingHealth cluster, Sengkang General Hospital was officially opened by PM Lee Hsien Loong on 23 Mar 2019, and is co-located with a community hospital for seamless care. With 1000 acute beds and 400 community beds, it caters to the north-western population within Singapore.
The Department of Radiology, SKH offers all Diagnostic and Interventional Radiology investigations along with Nuclear Medicine and Nuclear Cardiology investigations. Despite being a relatively new hospital, SKH DOR has effectively responded to the growing number of radiological examinations.
A few highlights at the DOR include the One-stop Thyroid Ultrasound and Biopsy Service, One-stop Joint Injection Service and the One-stop Breast Lesion Diagnostic and Biopsy Service. SKH DOR has also placed a DECT scanner in the Emergency Department to cater to trauma cases.
In keeping with the SingHealth spirit of teaching, SKH DOR teaches radiography students from Singapore Institute of Technology and Parkway College, and medical students from Duke-NUS Medical School, NUS Yong Loo Lin School of Medicine and NTU Lee Kong Chian School of Medicine.
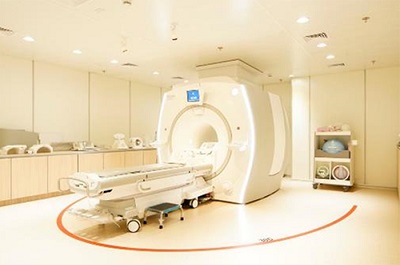
3T MRI machine. Photo courtesy of Sengkang General Hospital.
For appointments at SKH, call (65) 6930 6000.
KK Women’s and Children’s Hospital Department of Diagnostic and Interventional Imaging

The KKH building. Photo courtesy of KK Women’s and Children’s Hospital.
KKH is a 756 bedded- hospital and the national referral centre for high-risk obstetrics, gynaecological cancers, urogynaecology, paediatrics and neonatology. KKH operates a 24 hour Children’s Emergency service.

For appointments at KKH, call (65) 6225 5554.
National Cancer Centre Singapore, Division of Oncologic Imaging

The NCCS building. Photo courtesy of the National Cancer Centre Singapore.
The National Cancer Centre Singapore is a modern multidisciplinary cancer centre. Patients are treated in an outpatient setting, with some patients receiving inpatient treatment at SGH.
NCCS houses an imaging division dedicated to oncology, and holds joint boards with clinical service departments. NCCS also serves as a Breast Screen Singapore reading and recall assessment clinic.
For appointments at NCCS, call (65) 6436 8000.
National Neuroscience Institute, Department of Neuroradiology

NNI Department of Neuroradiology. Photo courtesy of the National Neuroscience Institute.
National Neuroscience Institute (NNI) provides comprehensive 24-hour MRI and rapid CT neurodiagnostic services, including CT angiography and CT perfusion.
NNI is one of the few sites in Singapore with round-the-clock coverage for neuro-angiographic and neuro-interventional services, including endovascular therapy for acute stroke. “Seeing patients with acute stroke recovering from neurological deficits post-thrombectomy is the most rewarding experience that keeps us going, despite sleepless nights”, says Dr. Kee Tze Phei, a neuroradiologist at NNI.
NNI Neuroradiology team has strong working relationships and their core strength lies in mutual respect, having open communication and a flat hierarchy. The team comprises neuroradiologists, nurses with subspecialty skills in neuro-interventional procedures, allied health professionals including radiographers, MR physicist and ancillary staff.
NNI practices daily review sessions which provide a conducive platform for case discussion and learning. In addition, regular journal clubs and clinico-radiology multidisciplinary meetings including neuro-ophthalmology, neuro-vascular, neuro-pathology and neuro-oncology meetings are well-attended and provide great learning opportunities for residents.

NNI Department of Neuroradiology. Photos courtesy of the National Neuroscience Institute.
For appointments at NNI, call (65) 6357 7153.
National Heart Centre Singapore, Department of Cardiac Radiology
The Department of Cardiac Radiology at the National Heart Centre Singapore provides a comprehensive range of radiological examinations, including general radiography at the outpatient clinics, cardiac and vascular interventional imaging and multi-slice computed tomography (CT) cardiac imaging.
NHCS also performs procedures such as angiography, percutaneous transcatheter coronary angioplasty, right heart catheterisation, cardiac valve repair/ replacement and electrophysiology procedures.
For appointments at NHCS, call (65) 6704 2000.
The SingHealth MRI Centre, located at Dunearn Village (Level 3), offers a wide range of MRI scan services in a comfortable and welcoming environment. Our centre is equipped with the latest MRI scanners, designed to produce clear, high-quality images while keeping scan times as short as possible.
As a SingHealth patient, your doctor may refer you to the SingHealth MRI Centre for your MRI scan. You can expect the same high standard of care and imaging quality, with the added benefit of shorter waiting times.
++ MRI services at this centre is currently offered to patients of Singapore General Hospital. It will be extended to patients of other SingHealth institutions in 2027.


Related Conditions & Treatments
Click for more information on the disease or condition.
Looking for other conditions?
Nuclear Medicine (NM) services are available at all SingHealth restructured hospital campuses. The Department of Nuclear Medicine and Molecular Imaging (DNMMI) in SGH handles all NM studies within the main department at SGH, and also provides imaging services to other campuses, including CGH, KKH, SKH and TTSH (part of the National Healthcare Group).
DNMMI performs at least 70 therapies per month including radioactive iodine therapy for benign and malignant thyroid conditions, selective internal radiation therapy (SIRT) therapy for malignant hepatic conditions, peptide receptor radionuclide therapy (PRRT) for neuroendocrine cancers, and prostate specific membrane antigen (PSMA) therapy, Radium-223 therapy and radiosynovectomy.
DNMMI performs approximately 450 general nuclear medicine scans and 85 PET-CT studies per week.
Dr Xie Wanying, a nuclear medicine physician, says, “We are privileged to be working in Singapore General Hospital, where our leaders listen to our voices. At our department, we have had the opportunities to introduce modern imaging studies such as I-123 ioflupane, F-18 flutemetamol, as well as novel therapies supported by well published results, such as PRRT and PSMA therapy.” She enjoys coming to work daily as there is a safe and conducive working environment with friendly co-workers without rigid hierarchy within the department. Everyone is free to express their opinions, especially with regards to ideas on improving patient safety and workplace efficiency.
DNMMI holds weekly peer review learning sessions, weekly resident teaching sessions and monthly journal club meetings.




















