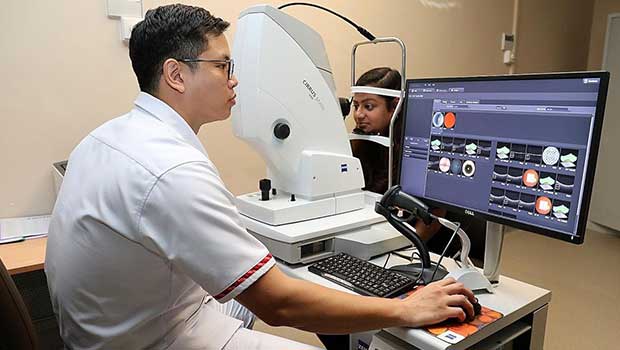
Enrolled nurse Abel Kwan (far left) using a specialised camera, known as a Fundus, at a mock screening session with the Selena+ AI. The system will address the need for increased manpower to tackle diabetes and related eye diseases.ST PHOTO: GIN TAY
Self-learning retinal screening tech cuts time needed to spot signs of diabetic eye disease
Imagine a future where the results and analysis of an eye scan can be produced in three minutes instead of an hour, and where even people in remote, rural communities can receive access to early screenings to prevent diabetic blindness.
These options may soon become realities, thanks to a state-of-the-art artificial intelligence (AI) software system, Selena+.
The deep learning system was jointly developed by a research team from the Singapore National Eye Centre's (SNEC) Singapore Eye Research Institute (Seri) and the National University of Singapore's (NUS) School of Computing.
Licensed to local start-up EyRis, the system is trained to analyse retinal photographs for signs of diabetic eye diseases in a fraction of the time it currently takes humans.
Selena+, which stands for the Singapore Eye Lesion Analyser Plus, does this by scanning the photographs for signs of three diabetic eye diseases.
These are: yellow and red lesions in the retina, a sign of diabetic retinopathy; an abnormal cup-to-disc ratio, a sign of glaucoma; and yellow lesions in the macular, a sign of age-related macular degradation.

Diabetic retinopathy, a major consequence of diabetes, is the leading cause of vision loss in working-age adults worldwide, which can result in blindness.
Currently, such analysis is done by trained readers in the SNEC Ocular Reading Centre (SORC) and at another centre in Tan Tock Seng Hospital.
The work is tedious, tiring and time-consuming.
SORC's senior manager Haslina Hamzah, who is also a founding member of EyRis, said her centre receives more than 4,000 images a day - all of which need to be processed by just eight to 10 staff who grade eye conditions.
These graders sit in a darkened room staring at retinal images on a screen, which they need to scan for abnormalities. They are typically not allowed to work for more than half a day as the job is too strenuous.
The images currently go through up to three levels of checks.
Primary graders are the first to take a look at an image after it has been sent to SORC. Ms Haslina said that around half of all images at this level typically turn out to have no abnormalities.
Images with abnormalities, as well as 10 per cent of the "normal" images, are then sent to a group of secondary graders.
If the primary and secondary graders disagree in their analysis of an image, it will be sent to an ophthalmologist. Only about 5 per cent of such images reach this stage, said Ms Haslina.
Selena+ is set to replace the role of the primary graders.
The system will address the need for increased manpower to tackle diabetes, the world's fastest-growing chronic disease.
Preliminary tests have shown Selena+ can cut the time that it takes for a report to return to a patient with "normal" results to just three minutes, down from one hour.
EyRis chief executive Lai Teik Kin said his company hopes to improve Selena+ so that future patients can receive their results almost instantaneously.
He added that the AI has proven itself "as good as a trained grader, if not better" during tests.
"Humans are inconsistent, but AI is consistent and doesn't tire," he said.
As a deep learning system, Selena+ "learns" and improves itself through experience, which means that the more images it has in its training dictionary to learn from, the more accurate it becomes.
The program was able to benefit from the large number of data sets - more than half a million - made available to it through the Singapore Integrated Diabetic Retinopathy Programme. The programme, which was started in 2010, allows patients to be screened for signs of diabetic eye disease.
Mr Lai, who is also chief executive of healthcare company Novahealth, said Selena+ is pending regulatory approval from the Health Sciences Authority before being rolled out across Singapore.
And when it does, it will be the first AI product in the world to be used by a national healthcare system for screening.
Ms Haslina said she hopes that Selena+ will be used in other Asian countries as well.
During screenings with Selena+, a type of digital camera equipped with specialised lenses - known as a Fundus camera - takes images of patients' eyes. The images will be downloaded on a computer that has Selena+ installed, after which the AI will make its assessment.
Mr Lai said he is seeking approval for Selena+ with other regulatory authorities around the world. He added that the AI - as well as the software responsible for its interface, Eyescan - can be adapted for different cultures and languages.
The concept of the Selena+ program was conceived in the 1990s by Professor Wong Tien Yin, who is currently medical director of SNEC, and two professors at NUS' School of Computing: Dr Wynne Hsu, who is now deputy head at the department of computer science, and Dr Lee Mong Li, now a professor of computer science.
The three of them are also founding members of EyRis.
Due to technological limitations and a lack of clinical screening results at the time, initial software prototypes were unable to reach the required levels of accuracy.
Seri's Technology Development and Commercialisation team, headed by Dr Danny Belkin, assisted the researchers with essential commercialisation aspects such as regulatory documentation and finding a multinational corporation to which it could license the technology.
Seri's team also linked Dr Hsu and Dr Lee with Novahealth, which helped to create Eyescan, the software used to interface with Selena+.
The various parties from SNEC, NUS and Novahealth then came together to form EyRis, to which Selena+ and Eyescan were licensed.
Dr Belkin said: "There are huge markets where there are just not enough (trained graders) and the scalability of an AI solution can solve a lot of problems... that's why this is a very exciting technology (and) we're very excited about it."
SERI'S TEAM WORKING ON OVER 100 PROJECTSSelena+ is just one of more than 100 projects that Seri's Technology Development and Commercialisation team has been working on since it was formed in 2012. They include: The team, which includes members with business and science experience, has three main roles: It also works with industries to bridge the gap between academia and industry. There are around seven main steps involved in the commercialisation process, from checking to see if there are any patents for similar projects and assessing the regulatory hurdles before researchers go through a prototyping phase. The product may also undergo human trials before it is introduced to the public. |



















