Harnessing the potential of 3D printing to take personalised medical services to the next level
As hospitals transform processes to deal with the challenges of an ageing population, adopting hightech initiatives to aid their efforts is advancing quickly.
At Singapore General Hospital (SGH), a 3D Printing Centre has been established, with the initial focus on producing 3D-printed patient-specific 3D models to help in pre-surgical planning and rehearsal of uncommon and complex operations. “SGH is harnessing the potential of 3D printing and expanding its use to achieve better patient care, starting with the launch of our very own 3D Printing Centre in SGH,” said Dr Mark Tan (below), Clinical Lead, 3D Printing Centre, SGH, and Consultant, Department of Diagnostic Radiology, SGH. “Currently, 3D models allow surgical teams to rehearse complex cases, as well as to pre-size and pre-shape implants to the patient’s anatomy before operations to improve their fit, patient outcomes and to decrease operative time.”

Indeed, said Dr Tan, requests to turn scans into 3D models are rising, either for surgical planning or implants. “We’ve been utilising 3D-printed models and implants, as well as performing research and development, in clinical 3D printing for a number of years as we see potential to improve patient care. One example is the 3D-printed custom bioresorbable implants, which give patients new treatment options,” he added.
Sunken chest

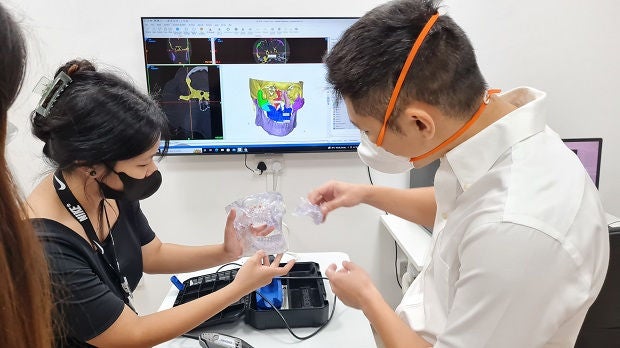
<<The 3D models use colours to better differentiate parts of the bone structure>>
In December 2021, SGH pioneered a treatment using a 3D-printed implant on a 20-year-old man with a condition known as pectus excavatum* or sunken chest.
He was born with a chest that curved inward from the top to the bottom, preventing both lungs from expanding fully, said Dr Chew Khong Yik (below), Senior Consultant, Department of Plastic, Reconstructive and Aesthetic Surgery, SGH. The deformity also pushed his heart against his left lung.

The patient first underwent a traditional treatment to insert a stainless steel bar into his chest to push it outward. His extensive deformity, however, meant that the lower part of his chest still curved inward. “We could have used a fat graft but, in a chest, it can be pulled down by gravity. When the patient runs or marches, the graft may move up and down, which can look unsightly,” said Dr Chew.
A second steel bar was not used on the lower deformity as the patient’s functions, like breathing, were not affected. Instead, a medical team led by Dr Chew turned to another method of addressing the concavity of the chest.
Working with local medical devices company Osteopore International, a bioresorbable polymer implant was developed for the patient. The custom-fitted porous structure embedded with bone marrow taken from the patient’s thigh bone acts as a scaffold for the patient’s own bone cells to regenerate and grow. Over two years, the implant will slowly dissolve, leaving the patient with a corrected chest that is made up of his own bone.
To create the 3D implant, the patient’s chest was first scanned in a CT scanner, and the image converted into a file that can be used to make the 3D model implant. SGH and Osteopore International worked closely using physical as well as virtual models to adjust and size the implant to be as near as possible to the structure of his body to reconstruct the chest deformity. The final implant was produced by Osteopore International for surgery.
“We believe our technique would enable more patients to come forward and seek treatment for this deformity. The implant is not permanent and is made using their own body tissue. With imaging-rendered technology, we can achieve perfect symmetry of reconstruction by using mirrorimaging techniques. With computer-aided design and manufacturing technology, we are able to create an implant that can fill the defect exactly,” said Dr Chew.
Creating a 3D model of the patient’s chest has other benefits, said Dr Tan. It can be used for planning and rehearsing the surgery, boosting the surgical team’s confidence in performing the operation. This allows the operation to go more smoothly, cuts surgery and anaesthesia times and results in a quicker recovery for the patient, he added.

<<Surgeons can plan and rehearse surgical procedures using 3D models, and this leads to better outcomes, says Dr Chew Khong Yik.>>
*What is sunken chest
Pectus excavatum or a sunken chest is not as rare a condition as some may think. It occurs in one in every 300 births. However, the severity varies, from the very mild, which does not need medical attention, to moderate and severe, where functional issues like breathing may be affected.
Of those born with the defect, 10 to 20 per cent of cases are severe. Men are more likely to suffer from social embarrassment as they have to bare their chests swimming or stripping down during National Service, for instance, and this can lead to anxiety and other mental health issues.
Severe spinal deformityA patient, Ms Chong Li Fong, was born with scoliosis, where the spine curves as a result of irregular growth during adolescence. The deformity, while visible, did not affect her until she hit her 50s, when she began to experience pain when sitting, standing and walking.
SGH sees an average of 500 scoliosis cases each year, of which 10 to 15 per cent require spine correction surgery. Many patients, however, hesitate to undergo the procedure because of potential surgical risks and complications such as paralysis. To overcome this, 3D-printed models to plan and prepare for complex cases like Ms Chong’s have now begun to be used.

With a personalised, life-size replica, the surgical team is able to see every detail of the spine and determine the safest way to perform the procedure. In Ms Chong’s case, Dr Reuben Soh (above), Senior Consultant,Orthopaedic Surgery, SGH, was able to use the model to show and explain to her the condition of her spine and what he would do during the procedure. This boosted her confidence and she agreed to the spine surgery. She had consulted other doctors before but was reluctant to undergo surgery as she was fearful of the risks.
“Using 3D technology, we were able to print out a model of the vertebrae and see which had worn out. During surgery, we need to push aside muscles, and sometimes it is difficult to know the exact location of each vertebra. With the help of the 3D model, we were able to carry out the surgery more quickly, neatly, optimally and safely,” said Dr Soh.
As 3D printing at SGH was still in its infancy then, Dr Soh enlisted the help of Associate Professor TooChow Wei, Senior Consultant,Department of Vascular andInterventional Radiology,SGH, to map Ms Chong’s spine by CT scan. The model was then sent to an overseas 3D printing company.
With the 3D model, the medical team was able to identify which of Ms Chong’s bones were deformed and where they were in relation to the spinal cord. Bones that were not located close to the spinal cord could be cut more quickly. Without the 3D print, a CT scan would have to be used during the operation, with time needed for the images to be processed into a 3D image. With the 3D model, surgery time was reduced by about two hours. Post-surgery, Ms Chong can stand straight and is 8 to 10cm taller than before. She goes about her daily activities without pain, and even takes hour-long walks with her father.
Dr Soh continues to work with Assoc Prof Too on developing 3D models of very complex spine conditions, as well as of spinal deformities caused by tumours.
What is 3D printing?

In 3D printing, thin layers of materials are fused, one at a time, from a digital file, to produce a three-dimensional object. The materials used in 3D printing range from plastics and carbon fibre to glass fibre and even chocolate and pasta. Three-dimensional printing has been applied in medicine since the early 2000s, with the technology first used to make dental implants and customised prosthetics. It has since evolved to produce bones, ears, exoskeletons, tissues and organs.
Get the latest updates about Singapore Health in your mailbox! Click here to subscribe.
Contributed by




















