SingHealth Institutions will NEVER ask you to transfer money over a call. If in doubt, call the 24/7 ScamShield helpline at 1799, or visit the ScamShield website at www.scamshield.gov.sg.
Extracorporeal Shockwave Therapy
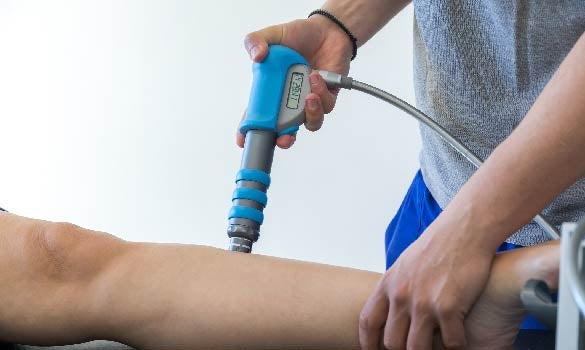
Following various studies into the effects of extracorporeal shockwave therapy (ESWT) on the musculoskeletal system, it has been increasingly used worldwide in treating common sports injuries. With its efficacy and very minimal adverse effects, it presents a promising treatment option for conditions such as proximal plantar fasciitis and tendinopathies.
Extracorporeal shockwave therapy (ESWT) was first used clinically in the 1980s for the treatment of renal calculi. Its effects on bones were first investigated due to the apprehension that shockwaves may damage the pelvic bone inadvertently during its use in the treatment of renal calculi. Surprisingly, it was found that whilst shockwaves had no considerable effects on intact bone, it may actually stimulate osteogenesis in fractures on animal models.
This led to the first studies into the effects of ESWT on the musculoskeletal system, which were for the fracture non-union of bones. Studies done showed healing rates of between 60 to 90%, depending on the site, type of fracture, time between trauma and ESWT treatment, size of the fracture gap, and adequate stabilisation and immobilisation of the lesion post-treatment.
SHOCKWAVE TYPES
There are currently two major types of shockwaves used in ESWT, focused shockwaves and radial shockwaves.
Focused shockwaves have a single pulse, with an abrupt and nearly discontinuous change in pressure, travelling faster than the speed of sound through the medium it is propagating through (see Figure 1).
They are generated by electrohydraulic, electromagnetic and piezoelectric devices. They concentrate the shockwave energy on a well-defined point of the target tissue, with varying focal volume, depth of penetration, level of energetic flux density and total energy administered.
Radial shockwaves are sound waves whose physical properties significantly differ from those of focused shockwaves, with a slower rise time and a lower energy level (see Figure 2).
The use of focused shockwaves, especially at high energy levels, requires accurate identification of the area to be treated with radiographic or ultrasound guidance to avoid damage to the surrounding tissue and optimise treatment efficacy.
Currently, ESWT has been used for a multitude of musculoskeletal conditions seen at the Changi General Hospital Sport & Exercise Medicine Department, with the most common being proximal plantar fasciitis, followed by various tendinopathies such as lateral epicondylitis (tennis elbow), patellar tendinopathy and calcific tendinopathy of the shoulder. |

COMMON CLINICAL APPLICATIONS
Plantar Fasciitis
Plantar fasciitis is the most common cause of plantar heel pain. Contrary to its name, plantar fasciitis is currently not thought to be due to an inflammation process, but likely secondary to myxoid degeneration, microtears in the fascia tissues and collagen necrosis.
Studies have shown that ESWT has a success rate ranging from 34 to 88%, depending on the treatment protocol, devices used and methodology. In our own departmental audit, two-weekly treatments with 2,000 pulses of focused shockwave therapy had a success rate of about 70%.
Tendinopathies
The second most common use of ESWT in the department is in the treatment of tendinopathies, including tennis elbow, patellar tendinopathy and calcific tendinopathy of the shoulder.
In vitro studies have shown an increase in the gene expression of collagen types I and III and TGF-β, followed by the production of nitric oxide (NO) and collagen synthesis in tendons subjected to shockwave therapy. It has been postulated that these mechanisms may play a part in the therapeutic effects seen by ESWT on tendinopathies. Studies have shown treatment success rates ranging from 68 to 91%, depending on the area treated, treatment protocol and device used.
There have been very minimal adverse effects reported for ESWT treatment, with the most common being transient pain after treatment, ecchymosis/ petechiae, and dyesthesia. The use of ESWT in the treatment of musculoskeletal disorders has gained traction worldwide due to its efficacy and minimal adverse effects, and can be considered for the aforementioned conditions. |
Dr Lim Ang Tee is a Sports Physician at Changi General Hospital. He has a keen interest not only in sports medicine but also in community health, chronic disease management and disability sports.
He was the Chief Team Physician for Team Singapore during both the Rio Paralympics in 2016 and Asian Para Games in 2018. Other than these appointments in sports medicine, Dr Lim is a designated workplace doctor, a Lasting Powers of Attorney certificate issuer and also on the panel of assessors for disability assessment for Eldershield application.
GPs can call the SingHealth Duke-NUS Sport & Exercise Medicine Centre for appointments at the following hotlines:
Singapore General Hospital: 6326 6060
Changi General Hospital: 6788 3003
Sengkang General Hospital: 6930 6000
Keep Healthy With
© 2025 SingHealth Group. All Rights Reserved.



















