Benign prostatic hyperplasia can often be managed effectively by GPs through medication review and lifestyle advice, though surgery may be considered in some cases. Find out more about the treatments available – including Rezum, a safe and effective minimally invasive surgical option.
INTRODUCTION
Benign prostatic hyperplasia (BPH) is a common condition affecting men above the age of 50. In BPH, the enlargement of the prostate gland results in lower urinary tract symptoms (LUTS), which are categorised into voiding and storage symptoms. Voiding symptoms include hesitancy, slow flow, intermittency and the sensation of incomplete voiding while storage symptoms include frequency, urgency and nocturia.
Areas of concern
The main concern for many men complaining of LUTS is prostate cancer. However, other concerns include the effect that BPH has on their quality of life and the possibility that it could be the cause of complications involving acute urinary retention.
While BPH has traditionally been managed in secondary care, the current availability of medical treatments means that the condition can now be managed effectively and safely in primary care.
For patients facing LUTS, GPs need to provide reassurance, appropriate lifestyle advice and a review of their medication and existing treatments.
TREATMENT TYPES
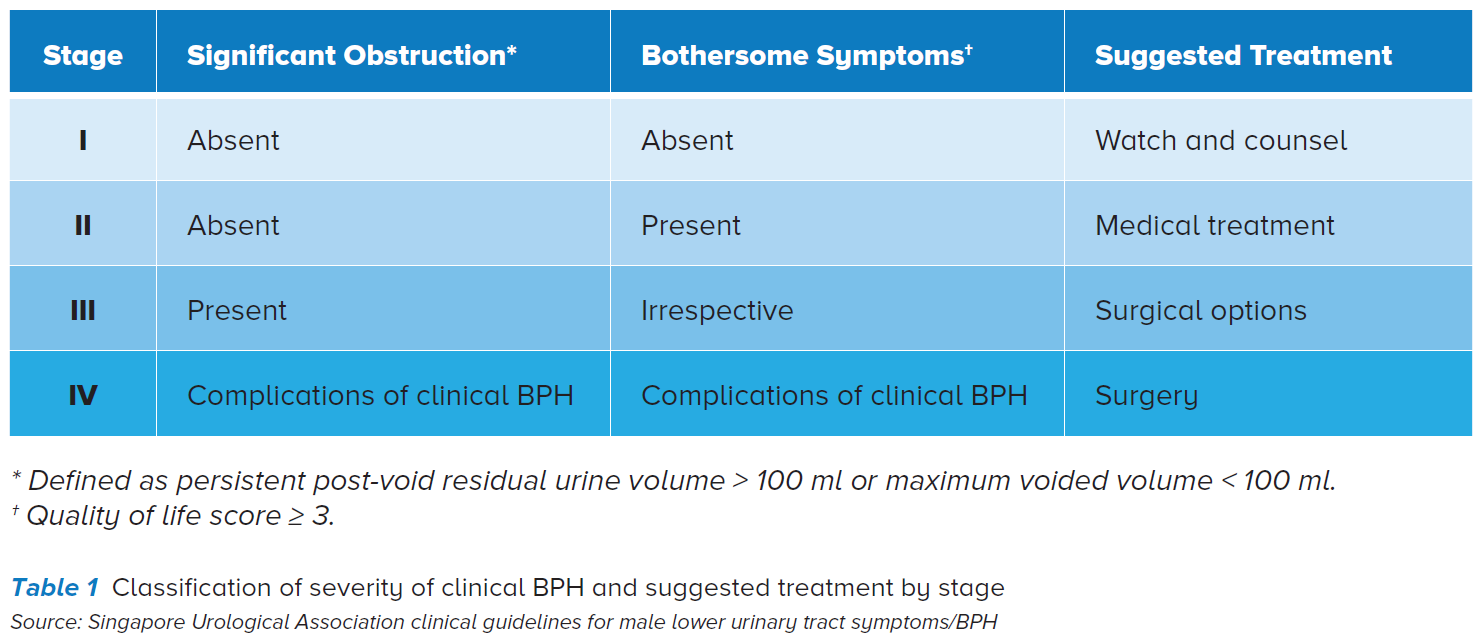
The various treatments commonly used to treat BPH include watchful waiting, medications and surgical options. Table 1 shows the different suggested treatments for the various clinical BPH stages.
A. Watchful waiting
Watchful waiting is suitable for patients with low-stage BPH. Those with no uncomfortable symptoms and no high post-void residual urine (PVRU) are ideal for watchful waiting.
Lifestyle adjustments will be recommended, such as the restriction of caffeine, alcohol and evening fluid intake, as these may improve storage symptoms such as urgency and nocturia.
B. Medications
Alpha-1 antagonists
These block the alpha-1 receptors in the prostatic urethra and around the bladder neck, resulting in a decrease in smooth muscle tone, thus reducing the dynamic component of prostatic obstruction.
Benefits
Alpha-1 antagonists improve the International Prostate Symptom Score (IPSS) by 30-40% and the flow rate by 20-25%. However, they do not prevent the progression of BPH. Patients usually experience the full therapeutic effect of alpha-1 antagonists within one week.
Side effects
However, there may be side effects such as postural dizziness and hypotension, which may lead to falls among elderly patients. Patients may also experience symptoms such as nasal congestion and abnormal ejaculation.
5-alpha reductase inhibitors
These block the conversion of testosterone to dihydrotestosterone, resulting in prostatic epithelial atrophy. This results in a decrease in prostatic volume, thus reducing the static component of prostatic obstruction.
Patients often experience full therapeutic effects only after six months of treatment and the efficacy is more pronounced in those with larger prostatic volumes. For prostatic volumes of less than 30 g, the efficacy is minimal.
Benefits
They have been shown to prevent BPH progression and decrease the incidence of acute urinary retention and BPH-related surgery for up to four years.
Side effects
The side effects include decreased libido, erectile dysfunction and gynaecomastia.
Combination therapy with alpha-1 antagonist and 5-alpha reductase inhibitor
Combination therapy can be considered among patients with prostate volumes of more than 30 g and who do not respond well to alpha-1 antagonist monotherapy.
Benefits
Combination therapy has the benefits of rapid onset of symptomatic relief by an alpha-1 antagonist and prevention of BPH progression by a 5-alpha reductase inhibitor.
Side effects
Side effects may also be more significant than monotherapy with either medication.
Phosphodiesterase-5 inhibitors
Tadalafil 5 mg daily may be considered for men with concomitant erectile dysfunction and uncomfortable LUTS.
C. Surgical options
The main considerations for surgery would include patients who have stage IV BPH and failed medical therapy (persistent uncomfortable symptoms despite medications or side effects from medications).
For surgical options, transurethral resection of prostate (TURP) has been considered as the gold standard. Although TURP is extremely effective in alleviating patients’ bladder outlet obstruction, it has common side effects and complications such as bleeding and sexual dysfunction (retrograde ejaculation).
Minimally invasive surgical treatments (MISTs) have been developed to reduce the morbidity of TURP and yet achieve good clinical outcomes in terms of improving patients’ LUTS. One of the newest MISTs is Rezum. Rezum employs a technology to convectively deliver to prostate tissue stored thermal energy in the form of water vapour (steam) created with radiofrequency current to produce instantaneous cell death in the targeted prostatic tissue. |
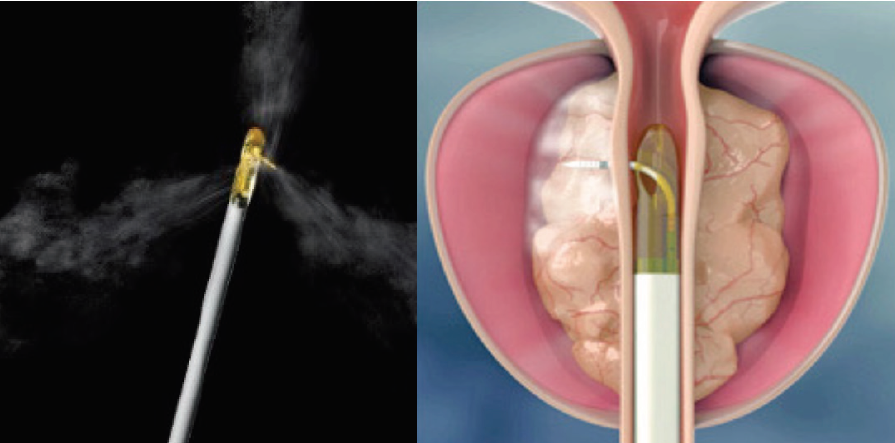
Delivery of targeted convective water vapour energy to the region of the prostate gland causing the obstruction
Reproduced with permission from Boston Scientific website bostonscientific.com
BENEFITS OF REZUM
In a randomised-controlled study by McVary et al., Rezum showed a significant improvement in LUTS (IPSS Score 47%, quality of life (QoL) 43%, Qmax 50%, Benign Prostatic Hyperplasia Impact Index 52%) through four years.
The re-treatment rate was also found to be low at 4.4% in four years.
Preservation of ejaculatory function
One major benefit of Rezum treatment is the ability to preserve ejaculatory function, which can be lost after TURP surgery.
This is especially important for younger men who require surgical therapy but would want to preserve their sexual functions. There is also less haematuria compared to post-TURP.
Convenience
- Rezum is also beneficial for patients who are not keen on long-term medications with their resultant side effects.
- It may also be more cost-effective than taking long-term medications.
- As this transurethral procedure takes only about 15 minutes and can be performed as a day surgery procedure, it obviates the need for overnight hospitalisation stays, which would otherwise be necessary for TURP surgeries.
- It can be done under general/regional anaesthesia and even with sedation or prostate block. Thus, this procedure may be suitable for patients who are not surgically fit for TURP.
Faster recovery
After the Rezum procedure, patients need to be on a urinary catheter for 7-10 days.
Most patients will be able to return to their normal activities after one to two weeks and will experience relief of symptoms one to three months after the procedure.
In the initial experience at Changi General Hospital (CGH), Rezum has shown to be a safe and effective procedure, improving patients’ LUTS. Patients who have undergone Rezum treatment have significant improvements in flow rate and symptom score, with no major side effects.
WHO CAN BE RECOMMENDED FOR REZUM
Rezum, being a minimally invasive surgical treatment, is a possible option for patients who:
- Have failed medical therapy
- Are not keen on long-term medications
- Are not comfortable with the invasiveness or side effect of sexual dysfunction that comes with TURP surgery
At the primary care level, patients who fit this profile can be recommended to choose Rezum as an option.
Background and medications Mr S is a 74-year-old with BPH who has been on medications since 2016. He has tried an alpha blocker medication (Terazosin) which caused him to have abnormal ejaculation. He has also taken finasteride which resulted in him having lethargy, low mood, decreased libido and erectile dysfunction. After stopping finasteride, the above-mentioned
symptoms disappeared. He has also tried another alpha blocker medication (Tamsulosin) which improved his urinary symptoms. He had missed his follow-up appointments for a few years and had consulted another urologist as he was experiencing giddiness after taking Tamsulosin. After stopping the medication, he had LUTS. He was offered surgical treatment (TURP), however he was not keen to undergo TURP due to the risks of haematuria and effects on his sexual health. He was interested in the Rezum procedure but it was not available in Singapore at the time. Referral to CGH Urology specialists He was then referred to the Urology specialist outpatient clinic at CGH in November 2020. He had experienced inconvenient LUTS of poor stream, incomplete emptying, terminal dribbling, urinary frequency, urgency and nocturia of five times per night. His prostate size was noted to be 48 ml with mild intravesical prostatic protrusion. His IPSS was
31/35 and QoL score was 6/6. His uroflowmetry showed a slow peak flow rate of 10.3 ml/s with a high PVRU volume of 155 ml. Positive outcomes He underwent the Rezum procedure in January 2021 after the procedure was introduced in Singapore. There was no postoperative haematuria and his urinary catheter was removed six days after surgery. After removal of the urinary catheter, he reported that his urinary stream was good. At about seven weeks post-Rezum, his urinary symptoms had improved significantly. His IPSS was 8/35, and QoL was 1/6. He reported that his urinary stream was very fast and his nocturia had decreased to one to two times per night. His peak flow rate was 13.7 ml/s (about 30% improvement) and had minimal PVRU volume of 27 ml. |
Dr Teo Jin Kiat is a Senior Consultant Urologist with the Department of Urology at Changi General Hospital. Aside from general urological diseases, his specialty interests include endourology and minimally invasive surgical techniques in the management of urinary stone disease and urologic cancers. Dr Teo is also actively involved in undergraduate and postgraduate medical education.
GPs who would like more information about this procedure, please contact Dr Teo at teo.jin.kiat@singhealth.com.sg.
GP Appointment Hotline: 6788 3003
