Transcatheter Aortic Valve Implantation (TAVI) has emerged as an alternative treatment of severe symptomatic AS in patients who are not suitable for conventional surgical aortic valve replacement due to high surgical risks.
The prevalence of aortic stenosis (AS) is increasing with the ageing Singapore population. It is estimated that moderate or severe aortic stenosis exists in 3% of patients more than 75 years old and 8% in those more than 85 years old.
The most common cause of Aortic Stenosis is degeneration of the native aortic valve in elderly patients. These patients often have multiple medical comorbidities and are at high risk for surgical aortic valve replacement, resulting in life-saving surgery being withheld. Less common causes of AS include rheumatic heart disease and bicuspid aortic valve.
The progress of AS is not altered with medical therapy. Once patients develop symptoms of severe aortic stenosis classically of chest pain, syncope and exertional dyspnoea, prognosis with medical therapy alone is grim with high mortality of 50% over 2 years.
Transcatheter Aortic Valve Implantation (TAVI) has emerged as an alternative treatment of severe symptomatic AS in patients who are not suitable for conventional surgical aortic valve replacement due to high surgical risks.
 TREATMENT OPTIONS FOR AORTIC STENOSIS
TREATMENT OPTIONS FOR AORTIC STENOSIS
Medical treatment for severe AS does not alter the poor prognosis and is of marginal benefits. Balloon aortic valvuloplasty carries significant procedural risks and is generally associated with restenosis of the aortic valve within 6 months of treatment.
The only effective therapy for AS is aortic valve replacement, which restores life expectancy to age-matched population without AS. Surgical aortic valve replacement typically with a bioprosthetic valve in the elderly patient is the gold standard of treatment in low surgical risk patients.
Patients are considered at high risk for open heart surgery either due to medical comorbidities or specific surgical technical difficulties, for example prior chest radiation therapy, patent coronary artery bypass grafts, and the presence of heavily calcified ascending aorta.
In such high surgical risk patients, TAVI can be a life-saving treatment for AS. The first implantation was by Cribier in 2002 and since then, the TAVI technology has taken quantum leaps with improvement in design and deliverability, resulting in better clinical outcomes with reduction of complications.
These advancements have resulted in the proliferation of TAVI worldwide, benefitting numerous severe aortic patients without surgical options who would otherwise face recurrent heart failure hospitalisation and certain mortality within a few years.
TRANSCATHETER AORTIC VALVE DEVICES AND IMPLANTATION PROCEDURE
At present, there are 2 established transcatheter aortic valve types for treatment of aortic stenosis:
1. The first is the
balloon-expandable stent valve design epitomised by the SAPIEN transcatheter heart valve (THV) by Edwards Lifesciences. The Edwards SAPIEN THV consists of three bovine-pericardial tissue leaflets sewn and mounted on a balloon-expandable stent frame.
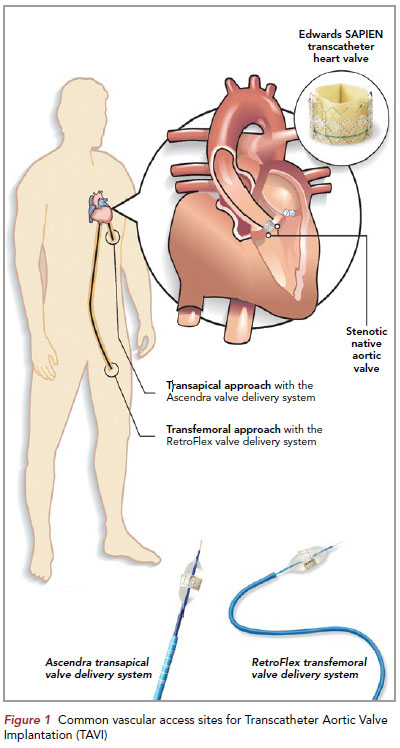
The stent valve is crimped onto a balloon on a valve delivery system. This valve is designed to be implanted from the common femoral artery or from the left ventricular apex if the femoral arteries are unsuitable (Figure 1). A support wire is positioned across the native aortic valve in the left ventricle.
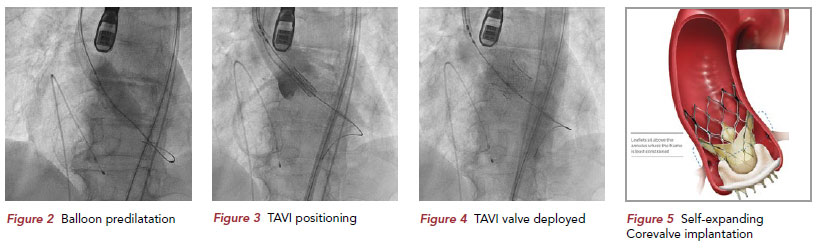
After initial balloon predilatation of the aortic valve (Figure 2), the stent valve is positioned across the native aortic valve on a support wire (Figure 3). The heart is then paced rapidly at typical rates of 180 per minute via a temporary pacing wiring placed in the right ventricle to reduce cardiac output, stabilising the THV position and allowing for accurate implantation of the THV by balloon inflation (Figure 4).
2. The second valve type is the
self-expanding stent valve typified by the Medtronic COREVALVE (Figure 5). This valve design is implanted via the transfemoral, subclavian or direct aortic approaches.
At the centre of the system is a self-expanding Nitinol stent frame which holds 3 bioprosthetic valve leaflets made from porcine pericardium. The Corevalve delivery system accommodates the bioprosthesis and is brought across the native aortic valve over a support wire. The delivery system is then slowly withdrawn to uncover and deploy the sheathed self-expanding stent across the native aortic valve.
VASCULAR ACCESS FOR TRANSCATHETER AORTIC VALVE IMPLANTATION
The Transcatheter Aortic Valve Devices are primarily designed for implantation percutaneously via the common femoral artery.
Most devices require the insertion of an 18 French arterial sheath which mandates that the common femoral arteries have at least minimal lumen diameter of 6 to 7 mm without severe vessel calcification or severe tortuosity.
Improvements in design have reduced the size of the delivery system and the femoral artery size requirement to 5 mm, with the smallest profile TAVI devices allowing more patients to receive transfemoral TAVI therapy.
The adequacy of femoral artery vascular access is best evaluated with a CT scan which is done as part of preprocedural evaluation. For patients with unsuitable femoral-iliac arterial access, alternative vascular access includes the transapical, direct aortic, subclavian approaches.
The transapical approach in which a 26 French vascular sheath is placed via the left ventricular a small left anterior thoracotomy at the fifth or sixth intercostal space. In contrast, direct aortic approach involves direct insertion of a vascular sheath into the ascending aorta via a small median sternotomy at the second intercostal space (Figure 1).
The left subclavian artery of an adequate size can be used for subclavian approach when the patient’s femoral-iliac arteries are of inadequate size. Regardless of the approach, once the vascular sheath is placed, a support wire can be placed across the native aortic valve for which to deliver the percutaneous valve to be implanted.
Once the percutaneous valve has been implanted, the vascular access can then be securely closed either by surgical repair or using pre-deployed percutaneous suture devices especially in the case of the transfemoral approach.
TAVI procedures can be done under general anaesthesia or local anaesthesia with sedation using the transfemoral approach.
The TAVI procedure is generally completed within one hour and patient brought to the intensive care unit for observation overnight. The patient typically will be transferred to the general ward for ambulation the following day and will be discharged from hospital within a week.
RESULTS
Large multicentre randomised controlled trials have established the benefits of TAVI in treatment of AS patients with prohibitive surgical risk and improvements of mortality and quality of life/symptoms compared to medical therapy.
Comparable results to surgical aortic valve replacement have also been found in high surgical risk AS patients treated with TAVI. Emerging trial data have suggested similar safety and efficacy of TAVI treatment of low- to moderate-risk AS patients.
However, until strong evidence becomes available, TAVI will remain an alternative to the gold standard SAVR therapy of AS only in high-risk AS patients.
COMMON COMPLICATIONS
Common complications of TAVI trials include periprocedural death (3-4%), stroke (5%), vascular complications (10%) and high-grade AV block requiring pacemaker implantation (10- 20%).
Leakage around the TAVI valve or paravalvular leak (PVL) causing aortic regurgitation can be caused by incomplete sealing of the aortic annulus by the TAVI valve from calcification, inaccurate positioning of the TAVI valve or improper sizing of the TAVI valve.
Significant PVL occurring post-TAVI can lead to increased morbidity from repeated heart failure hospitalisations and increased mortality, which emphasises the importance of preprocedural planning, valve sizing and accurate placement of the TAVI valve.
AT THE NATIONAL HEART CENTRE SINGAPORE
At the National Heart Centre Singapore (NHCS), TAVI has been performed in high-risk AS patients since 2009, with more than 200 patients treated.
These patients have high surgical risk with a mean society of thoracic surgeon (STS) score of 8.3% (> 8% being at high risk for surgery) or with surgical technical difficulties including porcelain aorta in 19.3%, patent bypass grafts in 19.3%, redo sternotomy in 12.1%; significant comorbidities including severe lung disease in 4.3%, chronic renal disease in 14.3% and advanced age/frailty in 19.3%.
TAVI was performed using the:
- Transfemoral approach in 75.7%
- Direct aortic approach in 3.6%
- Transapical approach in 20.7%
Procedural success was 91%.
Mean aortic valve pressure gradient at pre-TAVI was 46.7 mmHg and post-TAVI 18.2 mmHg during index hospitalisation, 12.0 mmHg at 1 month, 11.8 mmHg at 6 months and 10.9 mmHg at 1 year. Mean aortic valve area at pre-TAVI was 0.7 cm2 and post- TAVI 1.6 cm2 at 6 months and 1.6 cm2 at 1 year.
Moderate to severe paravalvular leak post-TAVI was 11.4% during hospitalisation, 10.7% at 1 month, 5.7% at 6 months and 2.1% at 1 year. Mean New York Heart Association (NYHA) class was 2.7 pre-TAVI, 2.0 at 1 month, 1.8 at 6 months and 1.9 at 1 year post-TAVI.
30-day complication rates include:
- Mortality (8.6%)
- Pacemaker implantation (6.4%)
- Stroke (2.1%),
- Valve embolisation (2.1%)
- Major bleeding/vascular complications (12.1%)
This compares favourably with global data on TAVI procedures.
CONCLUSION
The development of TAVI has made available a life-saving therapy for the otherwise inoperable severe AS patient. TAVI is a safe and efficacious alternative to surgical aortic valve replacement for treatment of high-risk, severe AS patients.
GPs can call for appointments through the GP Appointment Hotline at 6704 2222.
Asst Prof Ho Kay Woon is a Senior Consultant in National Heart Centre Singapore (NHCS). He sub-specialises in interventional cardiology with special interests in percutaneous coronary artery intervention, and percutaneous valvular therapy including transcatheter aortic valve implantation (TAVI).
Asst Prof Ho is also active in medical education. He is the Director of Medical Student Education in NHCS, with contributions to the teaching of medical students from Duke- NUS, Yong Loo Lin School of Medicine and Lee Kong Chian School of Medicine.
Read more on transcatheter aortic valve implantation (TAVI) procedure
here.
